What is Shigella?
Shigella is a Gram-negative, non-motile, non-spore-forming, rod-shaped bacterium capable of causing disease in humans. Disease occurs when virulent Shigella organisms are consumed and invade the intestinal mucosa, resulting in tissue destruction. Some Shigella strains produce enterotoxin and Shiga-toxin. Humans and higher primates are the only known hosts of Shigella. Depending on age and condition of the host, less than 200 cells can be enough to cause disease (FDA, 2012).
What causes the foodborne illness shigellosis?
Shigellosis is an infectious disease caused by bacteria of the genus Shigella. There are four different groups of Shigella species: Shigella dysenteriae (group A), Shigella flexneri (group B), Shigella boydii (group C), and Shigella sonnei (group D). S. sonnei causes most shigellosis illnesses in the developed countries, and accounts for approximately 70% of shigellosis cases in the United States. Conversely, S. flexneri is the prevalent species associated with illness in the developing world (CDC, 2009). The Centers for Disease Control and Prevention (CDC) estimated that Shigella causes over 130,000 cases per year in the US, which accounts for 1.4% of total foodborne illnesses (Scallan et al, 2011).
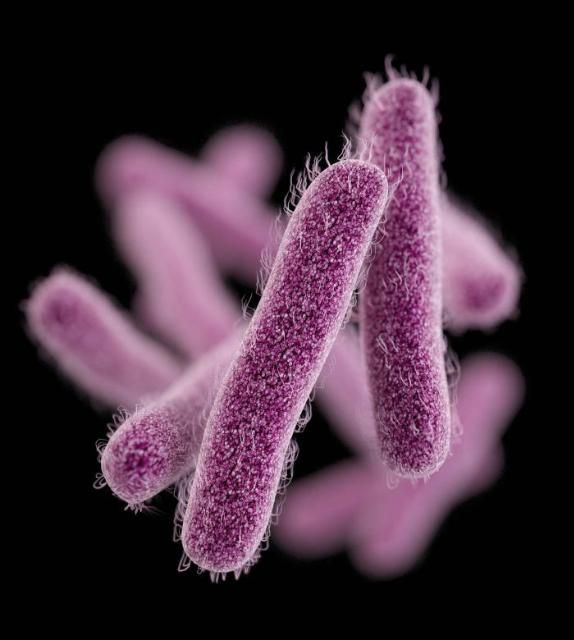
Credit: U.S. Centers for Disease Control and Prevention - Medical Illustrator
What are the symptoms of shigellosis?
Shigellosis is characterized in humans by sudden and severe diarrhea (gastroenteritis or bacillary dysentery), which is often bloody. Most infected people also develop fever and stomach cramps within 1–2 days after exposure to the bacteria. Symptoms typically last 5–7 days, and most shigellosis cases resolve without need for hospitalization. Shigella thrives in the human intestine and is commonly spread through both food and person-to-person contact. Some persons who are infected may show no symptoms at all, but may still pass the Shigella organism to others.
Long-term Effects of Shigellosis
Up to 3% of persons who are infected with Shigella may later develop chronic joint pain, swelling and irritation of the eyes, and sometimes painful urination. This is a reaction to the previous gastroenteritis and is called reactive arthritis. It is a rare autoimmune disease that can occur after a bout of gastroenteritis from Salmonella or Shigella.
How is Shigella spread?
Shigellosis typically occurs by fecal–oral contamination. Most Shigella infections are spread by stools or soiled fingers of an infected person to the mouth of another person when basic hygiene and handwashing are not properly done (for example, when people do not wash their hands with soap and water after using the restroom or changing a diaper). Shigella infections can be also acquired from consuming food contaminated by infected food handlers (through poor personal hygiene). In rare cases, swimming water in ponds, lakes, and pools can also spread Shigella if not properly treated and if enough water is swallowed. Such contamination may originate from sewage leaks or infected swimmers (particularly infected swimmers who have or recently have had diarrhea).
Tests and Treatment
Shigella is not a normal inhabitant of the human colon, but cultures are sometimes falsely negative. This is because Shigella shares several characteristics with normally occurring colon bacteria (native flora), making it difficult to isolate it from a stool specimen. Diagnosing Shigella as the causal agent of an illness requires laboratory testing to identify the bacteria in the stool of a possibly infected individual. Lab tests can also tell which species of Shigella are present to help determine which antibiotics are suitable for treatment.
What foods have been commonly associated with Shigella?
A wide variety of foods can be contaminated with Shigella. Foods that have been identified in Shigella outbreaks include salads (potato, shrimp, tuna, chicken, turkey, macaroni, fruit, and lettuce), chopped turkey, rice balls, beans, pudding, strawberries, spinach, raw oysters, luncheon meat, and milk. Contamination of these or other foods is through the fecal–oral route. This means the food has come in contact with water that has been contaminated, or has been handled under other unsanitary conditions. It is possible for any food that has been mishandled to become contaminated and spread the disease.
Prevention
The best was to prevent the spread of Shigella is through basic personal hygiene and frequent handwashing. You should wash hands with soap carefully, especially after going to the bathroom, before preparing foods, and after changing diapers. Toddlers and small children should be supervised for proper handwashing.
Other tips to prevent shigellosis are shown below:
-
Do not prepare food for others while ill with diarrhea.
-
Avoid swallowing water from ponds, lakes, or untreated pools.
-
Dispose of soiled diapers properly, and disinfect changing areas after using them.
-
When traveling in developing countries, drink only treated or boiled water.
How can you minimize the risk of shigellosis in your plant or establishment?
One of the most important sanitation steps to reduce the spread of shigellosis is the treatment of municipal water supplies. Water treatment for public consumption is a safe and highly effective preventative measure that has been in place for many years. Additionally, the treatment of sewage alleviates the spread of Shigella and many other disease-causing organisms, including Shigella. For this reason, use of municipal water supplies is recommended for all food-handling facilities.
Improved worker and facility hygiene at picking and packing facilities is a major step in preventing shigellosis caused by contaminated produce. To increase the safety of domestically produced foods, both the US Department of Agriculture (USDA) and the Food and Drug Administration (FDA) have established a hazard analysis and critical control points system (HACCP) for several sectors of the food industry. In hopes of further minimizing the risks of foodborne illness, the FDA has since considered establishing similar food safety standards throughout other areas of the food industry, including domestic and imported food products.
Sanitary conditions for food product receiving, handling, processing, and storage
The stringent requirements of the HACCP program have been argued as being too cumbersome or inappropriate for some food handling operations—specifically minimally processed foods. For these facilities, adoption of a program of general good manufacturing practices for food (GMPs), as defined by the FDA Code of Federal Regulations, Title 21, Part 110 (FDA, 2009), is suggested. An outline of such GMPs is available from the FDA Center for Food Science and Applied Nutrition and suggests the minimum general sanitation requirements for an FDA-inspected food handling and processing facility. To address any specific needs of an individual facility (such as for a particular procedural step or for the safe use of a particular piece of equipment), sanitation standard operating procedures (SSOPs) should also be developed and followed. Each facility should also be aware of and adhere to any appropriate state and/or local regulations. The Florida statues for retail food establishments can be found at http://www.leg.state.fl.us/statutes, Title 29: Chapter 381, and Title 33: Chapter 509.
The FDA Food Code outlines appropriate processing and cooking requirements for many food products processed in a retail facility. However, if certain high-risk food products (such as seafood, sushi, fresh juice, specialty meats, and others) are processed in the retail establishment, additional controls and the issuance of a variance (government permission for exception in the application of a given law, ordinance, or regulation) by the regulatory authority is required before processing can occur (Food Code 3-502.11).
Receiving
Specifications for receiving can be found in section 3-202.11 of the 2009 Food Code. The following guidelines cover the basic points to be addressed during receiving:
-
Potentially hazardous foods (PHFs) should be at a temperature of 41°F (5°C) or below when received, unless otherwise specified by law (e.g., milk, shellfish).
-
Raw shell eggs should be received at an ambient air temperature of 45°F (7°C) or less.
-
PHFs that are received hot should be at a temperature of 140°F (60°C) or above.
-
PHF should be received with no evidence of temperature abuse, such as thawing.
Handling and sanitation
Before and after use, clean and sanitize all cooking equipment, utensils, and work surfaces with a mild food grade bleach solution (100–200 ppm of free chlorine) or chemical sanitizers listed in 21 CFR 178.1010. Sanitizing solutions should be used in accordance with instructions on the EPA-approved manufacturer's label.
-
Let air-dry, if possible. Otherwise, use clean or single-use disposable kitchen towels / paper towels.
-
Use only potable water to wash and prepare food.
-
For display or service, select perishable foods last and put them away first.
-
Rinse and sanitize dishcloths often (or use single-use disposable towels) and use separate ones for each part of the kitchen.
-
Keep foods covered. Flies, other insects, or accidental splashing during preparation of other foods can spread contaminants.
Processing
The easiest way to prevent foodborne illnesses is to ensure that foods are thoroughly cooked. It should be noted that certain foods that are typically served uncooked, such as raw vegetables and fresh fruits, would obviously not benefit from a cooking process where none exists. For these items, other factors such as washing, sanitation, worker hygiene, and proper storage take on much greater importance. For specific recommendations, consult the 2009 FDA Food Code.
Storage
Once a product has been received and/or processed, it is usually displayed or stored. Some guidelines that will help prevent contamination at this time include the following:
-
Frozen food should remain frozen until it is used.
-
If frozen food is displayed in a refrigerated case, it should remain at or below 41°F (5°C).
-
Product must be cooled adequately; refer to sections 3-501.14 and 3-501.15 of the Food Code.
-
Hold cooked product above 140°F (60°C) while displaying and under 41°F (5°C) while storing.
-
Properly label all stored product.
-
Refrigerate at or below 41°F (5°C) or freeze at 0°F (-18°C).
-
Avoid cross-contamination: keep raw foods away from ready-to-eat foods while shopping, storing, and preparing foods.

Personal hygiene
The #1 method of avoiding contamination of food with viral, bacterial, and/or parasitic disease is for all food handlers to regularly and properly wash their hands.
When to wash hands
While regular handwashing is recommended, some events should always be followed/preceded by thorough handwashing with soap and warm water for 20 seconds:
-
Before handling, preparing, or serving food
-
Before handling clean utensils, or dishware
-
After using the restroom
-
After touching your face, cuts, or sores
-
After smoking, eating, or drinking
-
After handling raw meat—especially poultry
-
After touching unclean equipment, working surfaces, soiled clothing, soiled wipe cloths, etc.
-
After collecting and taking out the garbage
-
Before and after assisting someone with diarrhea, after cleaning the bathroom, and after changing diapers
Proper procedure for handwashing
-
Wet your hands with warm water.
-
Apply soap and wash your hands for 20 seconds. Pay attention to hard-to-reach areas like knuckle creases, between fingers, and under finger nails. Include the forearm past the wrist as you wash.
-
Rinse and then dry with a single-use paper towel.
Some other hygienic tips are:
-
Do not share food, drinks, spoons, or straws.
-
If you have a child in day-care who has diarrhea, inform the day-care providers so they can make sure germs are not spread to other children.
-
Do not let anyone who has diarrhea use a pool or swim in a pond while sick.
References
CDC. 2009. National Center for Emerging and Zoonotic Infectious Diseases: Shigellosis website. Last date of access: 20 May 2022. https://www.cdc.gov/shigella/
FDA. Bad Bug Book, 2nd Ed. Apr 2012. pp. 25–28. Last date of access: 20 May 2022. https://www.fda.gov/media/83271/download
Food and Drug Administration. 2009. Food Code 2009. U.S. Public Health Service. Accessed 20 May 2022. https://www.fda.gov/food/fda-food-code/food-code-2009
Mead, P. S., L. Slutsker, V. Dietz, L. F. McCaig, J. S. Bresee, C. Shapiro, P. M. Griffin, and R. V. Tauxe. 1999. Food-related illness and death in the United States. Emerging and Infectious Diseases 5:607–25. Last date of access: 20 May 2022. Available as .pdf at https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2627714/pdf/10511517.pdf
Ringrose J. H., A. O. Muijsers, Y. Pannekoek, B. A. Yard, C. J. P. Boog, L. Van Alphen, J. Dankert, and T. E. W. Feltkamp. 2001 Influence of infection of cells with bacteria associated with reactive arthritis on the peptide repertoire presented by HLA-B27. J. Med. Microbiol. 50:385–89.
Scallan et al. 2011. Foodborne illness acquired in the United States – Major pathogens. Emerging Infectious Pathogens 17:7–15. https://wwwnc.cdc.gov/eid/article/17/1/p1-1101_article
Stehulak, N. (n.d.). Ohio State University Extension fact sheet, HYG-5563-98. Shigella: An infectious foodborne illness. Last date of access: 20 May 2022. https://ohioline.osu.edu/factsheet/HYG-5563
The Florida Legislature. 2011. The 2005 Florida Statues. Last date of access: 29 March 2012. http://www.leg.state.fl.us/statutes