Florida is a tropical paradise that attracts marine enthusiasts and seafood lovers from around the world. Its extensive waterways not only offer unique areas for us to explore but also provide essential habitat for marine life. Although you cannot see them, marine bacteria are common throughout Florida waters. Marine bacteria play an important role in environmental processes by breaking down organic matter or providing food for larger organisms. There are many different species of bacteria that live in Florida waters. They are natural inhabitants of marine environments and live in and on many aquatic organisms.
Under certain conditions, one type of marine bacteria known as Vibrio is capable of causing wound infections and seafood sickness in people with weakened immune systems. People can encounter Vibrio if they expose an open wound to the water through activities like fishing and swimming or if they eat raw oysters and other raw seafood. Recently, the term "flesh-eating bacteria" has been used to refer to Vibrio. This description is false and misleading and causes unnecessary fear and panic. Vibrio should not keep Floridians and visitors from enjoying their favorite activities because Vibrio infections are rare and easy to prevent. Be aware of the hazards and follow a few simple safety guidelines to ensure that your time on the water is as safe and enjoyable as possible.
Hazards Associated with Vibrio Are Greatest:
- in stagnant, inshore waters and during warm, rainy months.
- for people who have weakened immune systems or underlying disease such as liver disease, diabetes, or hemochromatosis (iron overload).
- when a wound is submerged for a long period of time or an injury goes untreated.
- when an injury results from handling estuarine fish species, especially catfish, or shellfish, especially crabs and oysters.
- when people eat raw seafood, especially oysters.
Frequently Asked Questions
Vibrio and the Environment
What is Vibrio?
The name Vibrio refers to a large and diverse group of marine bacteria. Most members are harmless and can actually benefit the ecosystem by breaking down organic matter or providing food for larger organisms. However, some strains produce harmful toxins and are capable of causing a disease known as "vibriosis." About 15 species are known to infect humans, but two of particular concern are Vibrio vulnificus and Vibrio parahaemolyticus. The presence of these pathogens cannot be detected by the naked eye and specific laboratory techniques are necessary to confirm their identity (Drake et al. 2007).
Where and when are Vibrio bacteria found?
Vibrio bacteria naturally occur in coastal waters worldwide. They are not a result of pollution and can be present even if the water looks clean. Species that infect humans are most common in brackish environments, areas where fresh water mixes with salt water. Contrary to popular belief, Vibrio vulnificus and Vibrio parahaemolyticus are typically found in estuaries and bays rather than the beach or ocean due to their inability to tolerate high salt levels (Drake et al. 2007; Harbor Branch Oceanographic Institute 2021).
Though present in Florida waters year-round, Vibrio bacteria are most abundant from April to November, when temperatures are the warmest. These natural peaks correspond with an increase in human infections, which are usually highest during the summer months (CDC 2015). High concentrations can be encountered in stagnant inshore areas, especially near freshwater discharge sources.
Do I only need to worry about Vibrio in the summer?
In Florida's warm climate, Vibrio bacteria are present in brackish waters year-round. They are most abundant in the summer and early fall when the water is the warmest. People are also more likely to be in the water during these months. The combination of these factors contribute to a peak in reported cases during the summer (Weiss et al. 2011).
Why does Vibrio make us sick, but it doesn't make animals in the water sick?
Vibrio often attach to the bodies and shells of animals living in estuarine waters. As part of their natural microflora, which is the community of organisms that live in or on another living organism, these bacteria can benefit their hosts by providing food, breaking down waste and keeping them healthy. In the same way, microbes in the human gut help us absorb nutrients from food. Saltwater organisms are not infected, but can still transmit disease to humans. For example, shellfish can accumulate high concentrations of bacteria and cause disease if eaten raw. Fish, bait and tackle can also carry Vibrio, which can cause infections in anglers if they cut themselves or otherwise become exposed while fishing (Harbor Branch Oceanographic Institute 2021).
Are human activities like pollution responsible for Vibrio in Florida's waters?
No. Vibrio are a group of marine bacteria that naturally occur in local waters. They are not introduced by or associated with pollution. However, man-made events, like a discharge of fresh water, can alter Vibrio distribution by moving them into and allowing them to persist in areas where they normally do not occur (Harbor Branch Oceanographic Institute 2021).
Vibrio and Human Health
How common are Vibrio infections?
According to the US Centers for Disease Control and Prevention (CDC), Vibrio may cause up to 80,000 illnesses, 500 hospitalizations and 100 deaths in the United States each year. Only a small number of these illnesses are confirmed by laboratory testing and reported to public health agencies.
Most cases are reported from the Gulf and Atlantic coastal regions where the waters are warm and support both Vibrio and people enjoying an array of recreational activities. Infections resulting from Vibrio parahaemolyticus are the most common, but are usually mild and self-limiting. While infections from Vibrio vulnificus are rare, they are usually severe and have the highest fatality rates (CDC 2015; CDC 2014).
Vibrio has been in the news recently. Are illnesses in Florida new or increasing?
Vibriosis has likely occurred for hundreds of years but it has been documented in Florida only over the last 40 years. Over this time, the number of annual cases has increased (Weiss et al. 2011). This could be due to improvements in medicine and technology (facilitating diagnosis, reporting, and communication) as well as increasing tourism (more people in the water and eating more seafood meals means more people exposed). Currently, there is no evidence that Vibrio levels in the environment have increased.
Incidence of disease in Florida is typically higher than other parts of the country because of its warm weather, extensive coastline, and marine recreation. This may seem alarming at first, but infections are actually quite rare considering the millions of people that participate in water activities and consume local seafood each year.
How can people become infected?
According to the CDC, in order for infection to occur, pathogenic Vibrio strains must enter the body of a susceptible individual. This is usually a result of consuming raw and contaminated seafood, or prolonged exposure of an open wound in water containing Vibrio bacteria. Activities that may result in contact with these bacteria include fishing, wading and swimming, as well as cleaning and eating seafood, especially during summer months. The severity of disease depends on the type and amount of bacteria encountered as well as the individual's health (CDC 2014; Drake et al. 2007).
It is important to understand your personal risk for developing infection, which may be different from others around you. Be prepared and ensure that you have access to a first-aid kit when spending a day on the water. Remember, the best way to avoid infection is to prevent exposure in the first place.
Who is at risk for infection?
According to the CDC, most people are not at risk for developing illness. If Vibrio enters the body, a healthy immune system will combat infection, and it may cause only mild symptoms. However, people with weakened immune systems can develop life-threatening infections (CDC 2015). Several high-risk conditions that increase susceptibility include: liver disease, alcoholism, diabetes, hepatitis, hemochromatosis or iron overload, stomach disorders, HIV/AIDS, cancer, and long-term steroid use. Severe illness almost exclusively occurs in individuals who have these risk conditions (Drake et al. 2007). These patients are 80 times more likely to become ill and 200 times more likely to die. Though these cases are rare, they can be serious and progress rapidly (Oliver 2005). Seek treatment immediately if you suspect infection.
Is it safe for my children to go in the water?
According to the Florida Department of Health, infections from Vibrio vulnificus and Vibrio parahaemolyticus typically occur in patients that are middle-aged or elderly and have weakened immune systems. Children are not considered "high risk" for developing infections unless they have weakened immune systems due to underlying disease. While it is safe to swim in areas where Vibrio is present, it is never a good idea to expose unhealed wounds to the environment. Another species, Vibrio alginolyticus, is known to cause mild ear infections in children but can be easily prevented by cleaning and drying ears if they have water in them after swimming (CDC 2015).
Vibrio and Wound Infections
Is Vibrio really "flesh-eating"?
No. Vibrio cannot break down healthy, intact skin on contact, even if the skin is exposed for long periods of time. In order for infection to occur it must actually enter the body through prolonged exposure of an open, unhealed wound or be eaten, usually through raw seafood. Only after entering the body through these processes are they capable of causing disease in certain individuals. "Flesh-eating" is not a medical term and was likely derived from the fact that tissue death, or necrosis, can occur during advanced, late stages of infection around a wound if it is left untreated, especially in those with weakened immune systems (Oliver 2005).
What kinds of wounds can become infected?
Both previous injuries not fully healed—like cuts, sores, blisters, cracked feet, or broken skin—and new injuries—like scrapes from shells or punctures from fish spines, fishing hooks, and hidden debris—can open the door to Vibrio bacteria. Although wound infections can be caused by both species, they are commonly associated with Vibrio vulnificus. These cases are most commonly reported from fishermen and seafood processors, but they can occur in swimmers (Oliver 2006; Harbor Branch Oceanographic Institute 2021).
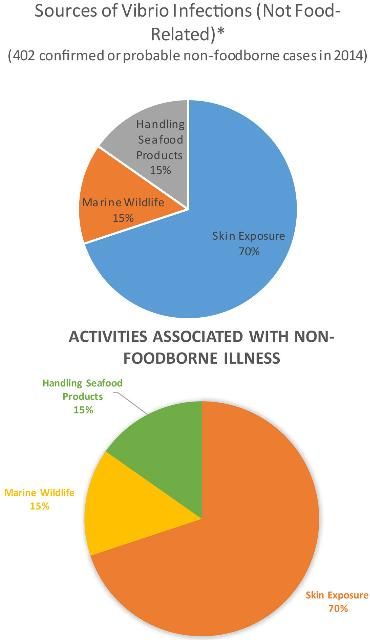
Credit: 2014 CDC COVIS Annual Summary
What are the symptoms of a wound infection from Vibrio?
Infections typically begin with swelling and redness of skin, followed by severe pain, blistering, and discharge at the site of the wound. If the infection progresses, especially in immune-compromised individuals, there can be tissue necrosis, fever, chills, low blood pressure, shock, and death may occur, especially if the infection spreads to the bloodstream.
Symptoms may arise within 1–3 days, but usually occur a few hours after exposure. Disease can progress rapidly and recovery is greatest when diagnosed early. Infections cannot heal on their own and require medical treatment such as antibiotics, aggressive wound care, or limb amputation. Seek medical treatment immediately if you suspect an infection (CDC 2015; Oliver 2005).
What should I do if I suffer a flesh wound during water activities?
Always have access to a first-aid kit and treat injuries as soon as they happen (WebMD 2021; Harbor Branch Oceanographic Institute 2021):
- Clean the wound thoroughly with soap and water, removing any foreign material or debris.
- Rubbing alcohol, peroxide, or antibiotic ointment should be used to reduce chance of infection. In some people, antibiotic ointments may cause a rash. If this happens, stop using the ointment.
- Cover the area with a bandage and prevent further exposure to environment. For a minor cut, remove bandage after a couple of days to promote healing.
- If the area becomes swollen, hot or very painful and you suspect infection seek medical treatment immediately.
For more complete advice, visit: http://www.webmd.com/first-aid/cuts-or-lacerations-treatment
Are there safety tips for preventing wound infections?
Remember, the best way to avoid infection is to prevent exposure by using the proper gear and safety practices (Harbor Branch Oceanographic Institute 2021):
- Contrary to popular folklore, it is never recommended to clean wounds by bathing them in seawater or other aquatic environments.
- Always access the water from a non-obstructed area where the bottom is visible. Be aware of hazards like submerged objects and wildlife.
- When wading, use puncture-resistant footwear with a good grip. Exercise caution on slippery surfaces like boat ramps, rocks, and kayak launches.
- Clean gear and wash off after being in the water, especially before handling food.
Are there specific safety tips for anglers?
Researchers at Harbor Branch Oceanographic Institute (2021) suggest:
- Always avoid or minimize handling fish whenever possible. This is not only beneficial for your health, but also for the fish.
- Keeping a fish in the water increases its chance of survival and reduces its ability to injure the angler. Decide ahead of time what you intend to keep and release unwanted fish right away.
- The proper use of a release tool can help remove hooks safely and quickly. If you plan to keep the fish, use a landing tool like Boga Grips or pliers to minimize handling.
- Circle hooks are recommended because they are more likely to catch a fish in the jaw, making removal easier. If the fish swallows the line or removal is too difficult, cut it as close to the hook as possible. Non-stainless steel hooks will likely fall out over time.
- If you cannot avoid handling the fish, use wet gloves to protect yourself. Be aware of areas that can cause injury like spines, barbs, and teeth. If you plan to keep the fish, place it on ice immediately.
- Always wash your hands thoroughly after fishing, especially before handling food. Be sure to clean your gear after each use with special care for sharp objects like hooks and knives.
- Live bait can also carry Vibrio. Use caution when hooking or handling, paying attention to areas that can inflict injuries like spines, shells, and claws.
- Bait buckets can be reservoirs for Vibrio because they accumulate bacteria from waste produced by the animals they contain. Do not overstock the container and be sure to exchange its water frequently. Use a hand net to retrieve bait and never submerge wounds.
- For shellfish harvesters: Always wear gloves and be cautious of sharp oyster shells, which can carry Vibrio. Commercial shellfish harvesters must follow guidelines in the National Sanitation Shellfish Program's Model Ordinance, which includes mandatory shellfish harvester educational training.
Vibrio and Seafood Sickness
Is it safe to eat local seafood?
Yes. According to the US Food and Drug Administration (FDA), the easiest way to prevent food-related Vibrio illness is to avoid eating raw seafood (FDA 2012). Because shellfish filter large quantities of water, bacterial cells can accumulate in their tissue. Seafood that has been properly cooked and handled should not contain Vibrio bacteria. Many hazards exist when you consume raw seafood, especially shellfish. If you eat raw fish or oysters get them from a reputable source to ensure they have been processed properly. If you are harvesting shellfish yourself, follow local guidelines such as when and where it is safe to collect. The Florida Department of Agriculture and Consumer Services (FDACS) provides information on shellfish harvesting management and shellfish harvesting open and closed areas (FDACS 2021).
People with weakened immune systems or those that are considered "at risk" for infection should not consume raw seafood (Wright et al. 2019).
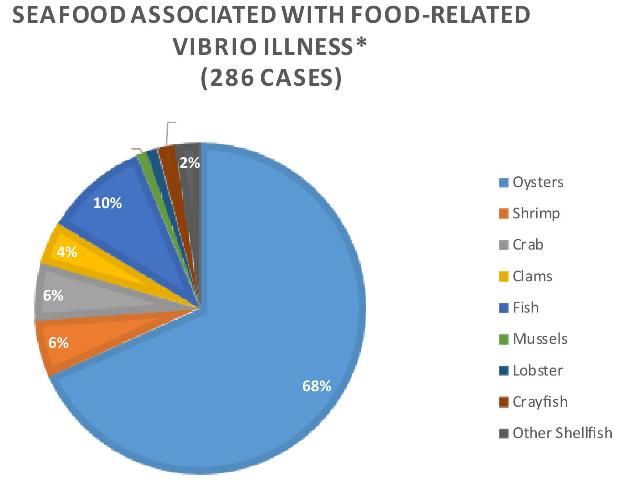
Credit: 2014 CDC COVIS Annual Summary
What are the symptoms of seafood sickness from Vibrio?
Symptoms include watery and/or bloody diarrhea, nausea, vomiting, abdominal cramps, headache, fever, and chills. Symptoms can occur anywhere from 4 to 36 hours after consumption, but generally start after about 15 hours. Illnesses typically last for 2 to 6 days; some are self-limiting and heal on their own over time, while those that are more severe can be treated with antibiotics (FDA 2012; Wright et al., 2019).
Most healthy people are not at risk of serious infection and will generally have mild symptoms. In individuals with weakened immune systems, disease can be severe or fatal if the infection spreads to the blood (causing septicemia or sepsis). Seek medical attention immediately if you have consumed raw shellfish and have any of these symptoms, especially if you are in a high-risk group (CDC 2015).
How can I keep from getting sick when eating seafood?
Heat from properly cooking seafood kills Vibrio and can eliminate the risk of illness. It is important to avoid cross contamination of raw seafood and juices with cookware, utensils, surfaces, or other food (Wright et al. 2019; American Liver Foundation 2021; Smith, Schmutz, Hoyle, and Hoover 2020).
- Thoroughly wash items that contact raw seafood with hot water and soap before they are used again.
- Keep food refrigerated if it will be used within 2 days and freeze items that will be stored for later.
- Seafood should be heated to at least 145°F (internal temperature) for at least 15 seconds.
- For shellfish still in the shell either: (1) Steam until the shells open, then continue cooking for 9 minutes. (2) Boil until the shells open and continue to cook for another 5 minutes. Never eat shellfish that do not open during cooking.
- For shucked oysters either: (1) Boil or simmer for at least 3 minutes or until edges curl. (2) Fry in oil at 375°F for at least 3 minutes. (3) Bake at 450°F for at least 10 minutes. (4) Broil 3 inches from heat for 3 minutes.
- For fish: Cook for 10 minutes per each inch of thickness at 450°F. This time can be doubled for unthawed, frozen fish.
Helpful Resources and Links
Florida Health Department: www.floridahealth.gov/diseases-and-conditions/vibrio-infections/vibrio-vulnificus
U.S. Centers for Disease Control and Prevention: http://www.cdc.gov/nationalsurveillance/cholera-vibrio-surveillance.html
Harbor Branch Oceanographic At FAU Vibrio Research and Safety Tips: https://www.fau.edu/hboi/research/ocean-health-human-health/microbiology/vibrio
For More Information on
Seafood
https://www.fda.gov/Food/ResourcesForYou/HealthEducators/default.htm
Florida Department of Agriculture and Consumer Services: https://www.fdacs.gov/Agriculture-Industry/Aquaculture/Shellfish
Fishing Safety
http://myfwc.com/fishing/saltwater/recreational/fish-handling/
Social Media Accounts
Florida Department of Health on Twitter — @HealthyFla and Facebook — https://www.facebook.com/FLDepartmentofHealth
Florida Sea Grant on Twitter — @FloridaSeaGrant and Facebook — https://www.facebook.com/flseagrant
References
American Liver Foundation. The Risk of Eating Raw Molluscan Shellfish Containing Vibrio vulnificus. Retrieved November 30, 2021, from https://www.issc.org/Data/Sites/1/media/Education/materials-for-web-posting-2020/issc-english-brochure-updated-version-2011.pdf
Centers for Disease Control and Prevention (CDC). 2014. "Cholera and other Vibrio illness surveillance (COVIS), summary data, 2014." Atlanta, GA: US Department of Health and Human Services. Retrieved November 30, 2021, from https://www.cdc.gov/nationalsurveillance/pdfs/covis-annual-summary-2014-508c.pdf
Centers for Disease Control and Prevention, National Center for Emerging and Zoonotic Infectious Disease, Division of Foodborne, Waterborne, and Environmental Diseases. 2013. "Vibrio Illness (Vibriosis), Vibrio parahaemolyticus." Retrieved June 5, 2015, from http://www.cdc.gov/vibrio/vibriop.html
Drake, S. L., A. DePaola, and L. A. Jaykus. 2007. "An overview of Vibrio vulnificus and Vibrio parahaemolyticus." Comprehensive Reviews in Food Science and Food Safety, 6(4): 120–144.
Florida Department of Agriculture and Consumer Services (FDACS) Shellfish. Retrieved November 30, 2021, from https://www.fdacs.gov/Agriculture-Industry/Aquaculture/Shellfish
Food and Drug Administration (FDA). 2012. Bad Bug Book, Foodborne Pathogenic Microorganisms and Natural Toxins. Second Edition. [Vibrio parahaemolyticus, p. 26; Vibrio vulnificus, p. 46]. Retrieved from http://www.fda.gov/Food/FoodborneIllnessContaminants/CausesOfIllnessBadBugBook/default.htm
Harbor Branch Oceanographic Institute at Florida Atlantic University. Vibrio Research and Practical Information. Retrieved November 30, 2021, from https://www.fau.edu/hboi/research/ocean-health-human-health/microbiology/vibrio
Oliver, J. 2005. "Wound infections caused by Vibrio vulnificus and other marine bacteria." Epidemiology & Infection 133(3): 383–391.
Schmutz, P.H., E.H. Hoyle, and A. Hoover. 2020. Foodborne Illness Related to Seafood. Clemson University Cooperative Extension, Home and Garden Information Center. Retrieved November 30, 2021, from https://hgic.clemson.edu/factsheet/foodborne-illness-related-to-seafood
WebMD. What Should I Do About Cuts, Scrapes, and Bites? Retrieved November 30, 2021, from http://www.webmd.com/first-aid/cuts-or-lacerations-treatment
Weiss, K.E., R.M. Hammond, R. Hutchinson, and C.G.M. Blackmore. 2011. "Vibrio Illness in Florida 1998–2007." Epidemiology and Infection, 139(4): 591–598.
Wright, A.C., R.M. Goodrich-Schenider, M.A. Hubbard, and K.R. Schneider. 2019. Preventing Foodborne and Non-foodborne Illness: Vibrio parahaemolyticus. FSHN0901. Gainesville: University of Florida Institute of Food and Agricultural Sciences. Retrieved November 30, 2021, from https://edis.ifas.ufl.edu/publication/fs146